13th Jul 2015
13th Jul 2015
Physical Therapy Treatment for Pelvic Dysfunction
Statistics say that 1 out of every 5 Americans (of every age) suffer from some type of pelvic floor dysfunction at some time in their life. Unfortunately, millions of Americans are suffering from pelvic floor dysfunction, yet for most, the disease goes unidentified and untreated. The problem is most folks don’t understand that there can be treatment for a condition that seems so personal, and well, internal. I’ve heard excuses like “I thought it was just part of getting old”, “I thought that’s what happens when you have a baby”, and “I was embarrassed” as reasons for not seeking treatment for pelvic dysfunction. There needs to be very real discussions and information available to patients who might be at risk for pelvic dysfunction so they understand they don’t need to suffer and that there are indeed treatment options available to them.
What is Pelvic Dysfunction?
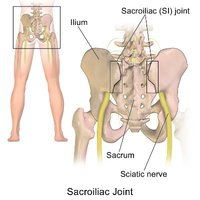
Pelvic floor dysfunction refers to a wide range of problems that occur when the muscles of the pelvic floor are weak, tight, or there is an impairment of the sacroiliac joint, low back, coccyx and/or hip joint.
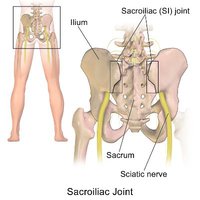
Sacroiliac Joint Impairment can lead to Pelvic Floor Dysfunction
The tissues surrounding the pelvic organs may have increased or decreased sensitivity and/or irritation resulting in pelvic pain. Many times, the underlying cause of pelvic pain is difficult to determine. These conditions may be due to infections (usually undiagnosed), pregnancy or childbirth, poor posture from chronic low back or SI dysfunction, trauma (e.g. bad fall), or a result of surgery. The pelvic floor is made up of muscles and other tissues that form a sling from the pubic bone to the tailbone. They assist in supporting the abdominal and pelvic organs, and help to control bladder, bowel and sexual activity.
When a person suffers from pelvic dysfunction, seeking the help of a physical therapist can help with the myriad problems that can occur including:
- Urinary urgency, frequency, or hesitancy, stopping and starting, painful urination, or incomplete emptying
- Constipation, straining, pain with bowel movements
- Unexplained pain in your low back, pelvic region, genital area, or rectum
- Pain during or after intercourse or orgasm
Physical Therapy Treatment for Pelvic Dysfunction
The mainstay of physical therapy for pelvic pain is hands-on treatment. That should include both external and internal techniques, although therapists will not use internal techniques until you are comfortable with them. External techniques may include: deep tissue massage often called “myofascial release” trigger-point therapy to release tight spots or “knots”, nerve release, and joint mobilization. Internal massage may also be used to release nerves and trigger points. Additionally, there are many tools a physical therapist may use to help patients relax their pelvic floor and relieve the pain directly.
Physical Therapy Tools for Pelvic Dysfunction
PTs also use a variety of devices to help you learn to relax your pelvic floor or to treat your pelvic pain directly.
- Biofeedback Devices use electrodes placed on your body (on the perineum and/or the area around the anus) or probes inserted in the vagina or rectum to sense how tense or relaxed your pelvic floor muscles are and display the results on a computer or other device. These cues can help you learn to relax those muscles.
- Electrical Stimulation stimulates your pelvic floor muscles directly through a small probe inserted into the vagina or rectum. This may help desensitize nerves or even cause muscles to contract and relax. Stimulation through electrodes placed on your body may be used to calm pain and spasms.
- Interferential Therapy is a kind of electrical stimulation delivered from electrodes placed on the skin. The impulses “interfere” with each other at the point of pain deep in tissues and can replace and relieve the sensations of spasm.
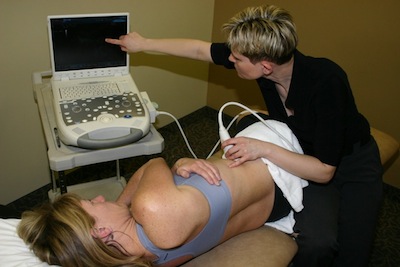
- Ultrasound uses high-frequency sound waves applied through a wand or probe on your skin to help treat pain. Therapeutic ultrasound uses sound waves to produce deep warmth that may help reduce spasm and increase blood flow or, on a non-thermal setting, may promote healing and reduce inflammation.
- Cold laser applies low-intensity laser light to the tissue and may help with pain, inflammation, and wound healing.
The problem the physical therapist faces is getting patients to seek treatment. Too many Americans don’t know or understand that they don’t need to just “live with” the problems associated with pelvic dysfunction and it is not in fact “just a part of aging.” Let’s provide the support needed to empower patients to seek help.